Mammary stem cells challenge costly bovine disease
Secreted factors from bovine mammary stem cells carry multiple positive effects.
April 25, 2018
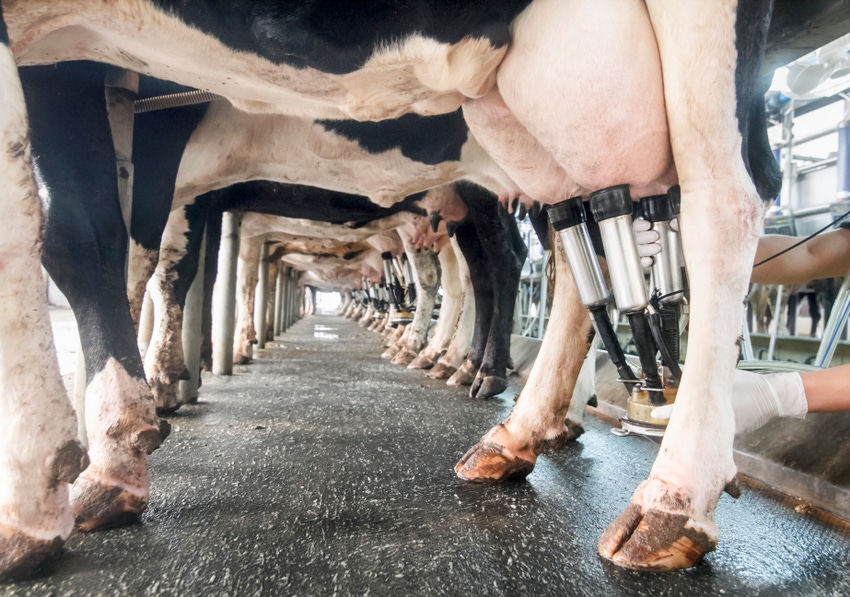
Mastitis is the most expensive disease in the dairy industry, as each clinical case can cost a dairy farmer more than $400 and damages both the cow's future output as well as her comfort.
Bovine mastitis is typically treated with antibiotics, but with the potential threat of antimicrobial resistance and the disease's long-term harm to the animal's teat, researchers at the Cornell University College of Veterinary Medicine are laying the foundation for alternative therapies derived from stem cells.
"Antibiotics can kill the bugs, but they don't help with regeneration of the damaged tissue," said Gerlinde Van de Walle, the Harry M. Zweig assistant professor in equine health.
Bovine mastitis damages the cow's mammary gland tissue when bacteria cause inflammation. The bacteria can enter the cow's teat when it comes in contact with a contaminated milking machine, a hand or bedding materials. This damaged mammary tissue contributes to milk production losses, quality concerns and increased labor costs, Cornell said.
"Bovine mastitis is the most costly disease in the dairy industry," said Dr. Daryl Nydam, professor in population medicine and diagnostic sciences at Cornell. "The second most costly is almost not worth mentioning in comparison."
According to the U.S. Department of Agriculture, 96.9% of dairy facilities use antibiotics to treat clinical mastitis cases. While effective against bacteria, antibiotics alone cannot restore the damaged mammary tissue. In a March 16 paper in Scientific Reports, Van de Walle and Nydam explored how the secretions of bovine mammary stem cells can encourage healing and regrowth of damaged tissue as well as rid the mammary gland of harmful bacteria.
"Even after the bug is removed with antibiotic treatment, the milk production will usually not go to its previous highest levels because of that damage to the tissues," said Van de Walle, lead author on the paper. "That's where this alternative therapy comes in."
Van de Walle and Nydam are the first to detail what bovine mammary stem cells secrete. Others have examined the secretome of stem cells from other species, but not bovines. "It's a brand new area of inquiry" that has led to a host of discoveries, Nydam said.
Their report shows that the secreted factors of these stem cells carry multiple positive effects, according to Cornell. They play a role in the formation of new blood vessels and promote the migration of cells, both of which are integral in healing tissue damaged by mastitis. Some secreted factors protect epithelial cells from damage caused by bacterial toxins, and others proved to be antimicrobial peptides that play a role in killing bacteria.
Van de Walle said, "Besides the tissue regeneration, it could also help the antibiotics work better, since they produce some of those antibiotic properties."
The researchers also found that the secreted factors were more effective against toxins produced by Gram-negative bacteria, which are generally more resistant to antibodies because of their thicker cell walls. The bacteria that cause bovine mastitis can be either Gram positive or Gram negative.
Food & Drug Administration-approved "intramammary antimicrobials are more effective against Gram-positive bacteria," Nydam said. "So, this would be a nice complement to that."
The paper is part of a concentrated effort for basic and applied science faculty to unite their research practices and address an important disease. Van de Walle's lab at the Baker Institute for Animal Health performs basic research on viral pathogenesis and stem cell biology, and Nydam is the director of Quality Milk Production Services, a program that addresses milk quality issues for producers, such as disease control and antibiotic use.
"Based on the positive effects of the bovine stem cell secretome we observed in the lab, we now have to take it to next level and test whether it also work in cows with mastitis," Van de Walle said.
You May Also Like



