Cornell researchers intend to extend this cost/benefit model to pork, poultry and beef production.
April 18, 2018
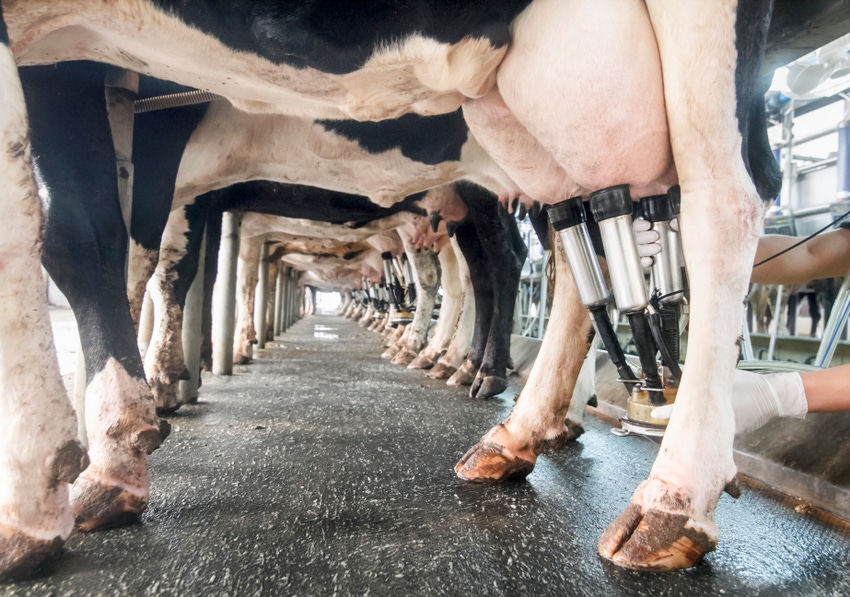
Dairy farmers use antibiotics to keep their herds healthy, but at the same time, these treatments may threaten public health through the creation of antibiotic-resistant bacteria. While the quantitative impact of such antibiotics on humans is not completely understood, a new Cornell University study has pinpointed the financial toll that eliminating antibiotic use would have on dairy farms -- a finding that could help guide regulatory policy.
“The Farm Cost of Decreasing Antimicrobial Use in Dairy Production,” published in PLOS One in March, shows that the cost of foregoing antibiotics on dairy farms would average about $61 per cow annually.
“If consumers or policy-makers wanted to implement antibiotic-free dairy production, it wouldn’t be a high cost for farmers, but it is feasible the farmers would ask to be compensated,” said Guillaume Lhermie, lead author and postdoctoral associate in the College of Veterinary Medicine at Cornell. ��“We wanted to see what we would win and what we would lose with this kind of regulation.”
The paper is part of a larger project, funded by the Academic Venture Fund of the Atkinson Center for a Sustainable Future, in which an interdisciplinary team is analyzing the impact of regulations that aim to curtail antimicrobial use in animal agriculture. The goal is to create a sustainable model that protects human and animal health as well as the livelihoods of farmers.
Because this issue has so many moving parts, the team is taking a systems approach that involves researchers in epidemiology, development sociology and agricultural and health economics, the university said in a "Cornell Chronicle" article.
“This antimicrobial resistant question is not only a basic science question,” said Yrjö Gröhn, the James Law professor of epidemiology and principal investigator. “You have to include these social concepts and people’s behaviors and economics if you really want to solve it and have an impact in society.”
To examine the effect of limiting the use of antibiotics in dairy production, Lhermie and Gröhn, along with Loren Tauer, professor at Cornell’s Charles H. Dyson School of Applied Economics & Management, modeled a dairy herd of 1,000 cows and factored in an average level of the nine most frequent bacterial diseases of dairy cows found in western countries. The researchers then calculated the net costs of prohibiting antimicrobial use as well as scenarios involving different treatment prices and milk withdrawal periods.
They determined that the cost of prohibiting antimicrobial use would, in many cases, be relatively minor — at $61 per cow annually — as long as regulations did not threaten the sustainability of milk production, the university reported.
The researchers intend to extend this model to include pork, poultry and beef production.
Gröhn emphasized that, in addition to such financial impacts, the team also took animal welfare into consideration. “You simply cannot decide not to treat animals for disease,” he said. “That is unethical.”
As the project moves forward, the team will zero in on the health consequences and the cost/benefit analysis of antibiotic use in animal agriculture.
“I think the real motivation for this study is that, as a society, we face difficult trade-offs. This sounds almost too literal, but (you know) the old saying, ‘There’s no such thing as a free lunch’? There’s no such thing as a free hamburger,” said Donald Kenkel, the Joan K. & Irwin M. Jacobs professor in policy analysis and management and co-primary investigator. So, we have to make this difficult choice.”
Kenkel continued, “We are worried about human health, we’re worried about animal health and we’re worried about agricultural productivity. How do we make trade-offs when policies that might be good for animal health and agricultural productivity might harm human health? That’s what the benefit/cost analysis is trying to come up with: a way to quantify those trade-offs.”
The project aims to educate policy-makers so they can make informed decisions about the sustainability of antibiotic use. Lhermie and Kenkel recently presented their research at the Society for Benefit-Cost Analysis annual meeting in Washington, D.C. The event — which addresses issues in energy, transportation, human health and agriculture — was attended by economists, academics and representatives from government and nongovernmental organizations.
“Antibiotic resistance doesn’t recognize any frontiers,” Lhermie said. “It can travel from the U.S. to anywhere in the world and vice versa, so there is a time scale but also a geographic scale to consider. We know there are going to be consequences in other countries, so there are questions of global governance which are also important.”
You May Also Like


.png?width=300&auto=webp&quality=80&disable=upscale)
